- Industry paid $8.2B to docs, hospitals last year (biopharmadive.com)
Drug and device makers collectively made nearly $8.2 billion in payments to physicians and teaching hospitals in the U.S. last year, according to data made public by the Centers for Medicare and Medicaid Services last week...Payments for research made up more than half of the total, which also includes money given to doctors and hospitals for expenses like travel, gifts, speaking fees and meals. The $8.2 billion recorded last year was a notch higher than 2015's total and $320 million more than 2014's figure...Among the ranks of big pharma...Roche spent the most — a princely $586 million in payments. Novartis and Pfizer were close behind with more than $475 million each, although both made more research-related payments than Roche did...The data gives a snapshot of the enormous sums of money paid by the drug and device industries to doctors and hospitals. Most of the money goes towards research, payments for things like enrolling patients into new clinical studies or study implementation. Research payments can also include direct compensation to doctors…CMS began tracking payments in 2013 as part of changes to federal law through the Affordable Care Act, with 2016 marking the third full year of the program...
- Change law and raise taxes to enable STPs to improve NHS, report urges (pharmaceutical-journal.com)
A lack of statutory power and severe underfunding are creating barriers to promising NHS reforms set out in sustainability and transformation plans (STPs), a think tank is warning...A report from the Institute for Public Policy Reform found that...44 regions in England had by and large correctly identified the right solutions, including moving care into the community and prevention...But there are several barriers that will prevent the ‘vision’ being realised, including a failure of leadership, the risk the NHS is being ‘engulfed by funding pressures’ and a lack of legal power to deliver the reform set out by the STPs...Among the IPPR recommendations is a call for the government to create a new ‘NHS tax’ by raising taxes for the highest paid to provide an extra £3.9bn a year to tackle the NHS ‘funding crisis’...In coming years, the NHS is facing a £22bn funding gap, which means limited resources are being spent maintaining the status quo rather than introducing a reform…There should also be changes to the law to better enable the pooling of budgets and commissioning functions locally and to give regional bodies a formal role in the system and put into effect place-based health and care...
- Pharmacy Week in Review: July 7, 2017 (pharmacytimes.com)
Nicole Crisano, PTNN. This weekly video program provides our readers with an in-depth review of the latest news, product approvals, FDA rulings and more.
- Shortages of Simple Drugs Thwart Treatments (wsj.com)ASHP - Drug Shortages List (ashp.org)
The scarcity of a simple medicine is complicating treatment for patients...Chronic drug shortages have burdened U.S. medical care for several years. Studies have estimated drug shortages add more than $400 million in annual U.S. health-care costs because hospitals and doctors are forced to seek more expensive alternatives, and health-care workers must spend extra time managing shortages...The shortages of low-cost medicines have been caused by a decline in the number of suppliers for certain products and failures by companies to build enough production capacity or meet manufacturing-quality standards...also...thinner profit margins for many older drugs reduce incentives for companies to invest in them...As a result of the shortage, doctors and hospitals are resorting to riskier and sometimes costlier treatments...FDA...said the agency works closely with manufacturers of drugs in short supply to help restore stocks, and asks other companies to increase production if they manufacture the same drug. The FDA says such efforts has helped cut the number of new shortages but can’t prevent all of them...
- Drugmakers and distributors face barrage of lawsuits over opioid epidemic (washingtonpost.com)
The companies that manufacture and distribute highly addictive painkillers are facing a barrage of lawsuits for the toll their product has taken on communities across the country as the worst drug epidemic in U.S. history continues to escalate...Within the past year, at least 25 states, cities and counties have filed civil cases against manufacturers, distributors and large drugstore chains that make up the $13 billion-a-year opioid industry. In the past few weeks alone, the attorneys general for Ohio and Missouri, along with the district attorneys for three counties in Tennessee, filed suits against the industry — and the attorney general for Oklahoma filed suit on Friday...The strategy echoes the effort against major tobacco companies in the 1990s and is born of similar frustration over rising death rates and the increasing costs of addressing the continuing public health crisis. After years of government and pharmaceutical firms failing to control the problem, some lawyers say the suits have the potential to force the industry to curb practices that contribute to it...Representatives of the companies deny wrongdoing and vow to vigorously defend themselves. They said they have taken steps to prevent the diversion of their drugs to the black market. Stemming the epidemic, they said, will take a coordinated effort by doctors, the industry, and federal and local government agencies..."As we look to prevent abuse and misuse in the future, it will require a forward-looking, systemic approach that calls on greater coordination and collaboration between health-care, law enforcement, and state and federal regulatory authorities," said the Healthcare Distribution Alliance, which represents companies that distribute drugs...
- Value-Based Care Increasing the Popularity of mHealth (ajpb.com)
Mobile health has become increasingly popular as the healthcare world moves towards value and away from volume, according to a new study by GBI Research. mHealth can connect patients with numerous healthcare services, while also collecting valuable data...This approach has already had an impact on the healthcare industry and numerous organizations are making investments in the technology. mHealth can also be used to encourage patients to adhere to their treatments, providing physicians with an additional way to communicate beneficial behaviors to their patients... advances in mobile technology, the expansion of communication, and the reduction in the cost of wireless technology...have huge potential to bridge the gap within existing healthcare systems, offering an alternative form of healthcare communication and treatment at a distance...The most important driver behind mHealth is the growing need for cost-effective ways to provide healthcare...Another important driver is the shift towards value-based care and reimbursement...healthcare providers are interested in helping patients achieve optimal outcomes rather than being incentivized to order more tests or perform more services.
- This Week in Managed Care: July 7, 2017 (ajmc.com)
Kelly Davio, Welcome to This Week in Managed Care from the Managed Markets News Network
- ICER to Work With VA on Drug Price Negotiations (raps.org)
In a first for the Institute for Clinical and Economic Review, which estimates the cost-effectiveness of drugs, the Department of Veterans Affairs Pharmacy Benefits Management Services office has agreed to use ICER drug assessment reports in drug coverage and price negotiations with the pharmaceutical industry...ICER says it will work with staff in the VA to integrate ICER reports into the VA formulary management process of evaluating the comparative clinical effectiveness and value of drugs...The VA requires that drug manufacturers offer a 24% discount off a drug’s average price or the lowest price paid by other (nonfederal) buyers, in addition to further discounts if a drug’s price outstrips inflation...The VA also directly negotiates lower prices with drug manufacturers, and with ICER’s help may establish a new norm for how the government can obtain lower-priced drugs...We will also assist the VA in exploring new ways it can use the reports to continue to provide a safe, effective and sustainable prescription benefit while more closely aligning a drug’s price with the value it provides to Veterans and the US taxpayer...ICER will also work with VA staff to develop options for using "value-based price benchmarks"...
- Praxsyn Corporation Acquires Nevada Pharmacy (finance.yahoo.com)
Praxsyn Corporation is pleased to announce that it has purchased through a newly formed subsidiary, Nevada Health Rx, Inc., the pharmacy license and all of the assets of Meds Direct Rx, a pharmacy located in Las Vegas, Nevada. The new pharmacy is about 8,000+ square feet of pharmacy and warehouse space, and includes a large loading dock and a secured yard to hold delivery vehicles...The total purchase price for the acquisition of the pharmacy was $120,000...This acquisition will allow us to sell a broader mix of products from a much larger facility than we have had in the past. Our focus is on filling prescriptions that have a 30 day pay cycle...Our focus...is on customer service to our patients, their doctors, the surgery centers and hospitals that will serve our patients...Headquartered in Las Vegas, Nevada, Praxsyn Corporation is a holding company that finds solutions to fit the needs and goals of medical professionals and their patients...
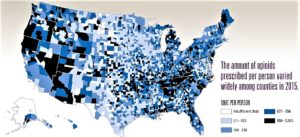
- Opioid prescribing is falling in the US, but not everywhere (philly.com)
Centers for Disease Control and Prevention...Prescriptions per capita, measured in morphine equivalents to account for various strengths and drug types, have declined steadily since their 2010 peak...Half the nation’s counties saw a decline (a quarter were stable) from 2010 to 2015. But there was wide variation, with providers in the highest-prescribing counties writing scripts for six times more opioids per resident than those in the lowest-prescribing counties...Nationally, the epidemic has been driven by high rates of addiction in more rural and white areas...Looking at county-level prescribing data helped CDC researchers to shed more light on some patterns of the painkiller epidemic. Counties with high rates tended to:
- Contain small cities or large towns (perhaps with pharmacies that drew residents from rural areas)
- Have higher percentages of white residents
- Have more dentists and primary-care physicians per capita
- Have more residents who were uninsured or unemployed
- Have more people with diabetes, arthritis, or a disability
But county-by-county analyses also illustrated how much is unknown about where and why opioids are given.