- CMS proposed rule expands telehealth for Medicare Advantage plans, beefs up payment audits (fiercehealthcare.com)
The Centers for Medicare and Medicaid Services issued a proposed rule...that would allow Medicare Advantage plans greater flexibility to offer telehealth benefits...The proposed rule would also update the Star Ratings methodology, streamline benefits for Dual Eligible Special Needs Plans and give auditors more latitude to recover improper payments. In doing so, the agency would codify multiple sections of the Bipartisan Budget Act of 2018 passed earlier this year...Perhaps the biggest change, which would take effect in 2020, would allow plans to offer "government-funded" telehealth benefits to all members whether they live in rural or urban areas. Beneficiaries could also receive telehealth services in their home rather than a medical facility...Industry groups have been clamoring for the government to rethink the limitations around telehealth reimbursement that limited services to rural patients...CMS suggested the telehealth provision may steer more Medicare enrollees toward MA, since traditional Medicare’s telehealth benefits are somewhat limited by location and clinical need...
- Jeff Sessions announces more prosecutors for crackdown on opioid providers (fiercehealthcare.com)
A day after President Trump signed a massive piece of legislation responding to the opioid crisis into law, the Department of Justice announced it's pouring even more resources into its crackdown on prescribers...Attorney General Jeff Sessions said his agency was creating a new Appalachian Regional Prescription Opioid Strike Force to focus on communities "hit especially hard by addiction and opioid fraud."...a dozen prosecutors and data analysts will operate out of hubs in Cincinnati/Northern Kentucky and Nashville, Tennessee, monitoring the Appalachian region for fraudulent opioid prescriptions by physicians...
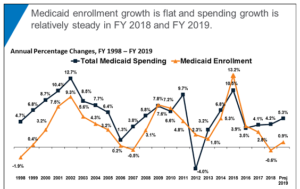
- Medicaid enrollment declines for the first time in more than a decade as strong US economy boosts income for poor Americans (cnbc.com)50-State Survey Finds Flat Medicaid Enrollment Tied to a Stronger Economy and New Eligibility Systems (kff.org)
Medicaid enrollment fell for the first time since 2007, declining by about 0.6 percent in fiscal year 2018, according to a new report from the Kaiser Family Foundation...States are budgeting for a "minimal" increase in enrollment of 0.9 percent in 2019, the report says..."States largely attribute the enrollment slowdown to a strengthening economy, resulting in fewer new low-income people qualifying for Medicaid," Kaiser says...Federal and state Medicaid spending still grew despite the drop in enrollment. Combined federal and state spending rose by 4.2 percent in fiscal 2018...The report also listed other factors that contributed to the rise in spending, including more expensive prescription drugs and states spending more money to treat substance abuse and mental health...
- As elections near, PhRMA’s lobbying spend on track for potential record-breaking year (fiercepharma.com)
Pharma has found itself an easy political target in Washington, and as a critical election nears, the industry's lobbying spend shows drugmakers are taking the threat of pricing reform seriously—and shelling out big-time to avoid it...Through the third quarter, pharma's top trade group PhRMA has spent $21.5 million lobbying lawmakers, a 10% increase over the same period last year...The figure puts PhRMA on track to beat last year’s spending of $25.43 million...
- Trump administration unveils plan to lower Medicare Part B prices by basing costs on other countries’ pricing (fiercehealthcare.com)Trump administration faces uphill battle in convincing provider skeptics to back new drug pricing plan (fiercehealthcare.com)
President...Trump...announced a new payment model that would more closely align the cost of Medicare Part B drugs with the prices paid for the same drugs in other countries...As they unveiled the "International Pricing Index" model, federal health officials projected the proposal could save Medicare more than $17 billion over the course of a five-year pilot. The Centers for Medicare & Medicaid Services currently pays the average sales price plus 6% for Part B drugs, and in the new proposal would instead pay a target price based on international prices and look to alternatives for the add-on fee...Medicare currently pays about 180% more than other countries for drugs in Part B, which includes pharmaceuticals that are administered in a clinical setting, HHS Secretary Alex Azar said. Through the IPI model, HHS is looking to bring that figure down to 126%.
- This Week in Managed Care: October 26, 2018 (ajmc.com)
Laura Joszt, Managing Editor at The American Journal of Managed Care. Welcome to This Week in Managed Care from the Managed Markets News Network...
- U.S. Health Chief Says Overdose Deaths Leveling Off (ktvn.com)
...health secretary Alex Azar says the number of drug overdose deaths has begun to level off after years of relentless increases driven by the opioid epidemic...Azar cautioned...it's too early to declare victory...However, he said that toward the end of last year and through the beginning of this year, the number of deaths "has begun to plateau."...provisional counts posted online by CDC show a slight leveling began toward the end of 2017.
- FDA’s Gottlieb ‘extremely worried’ on CAR-T reimbursement (biopharmadive.com)
Food and Drug Administration Commissioner Scott Gottlieb stressed the need for reform on the reimbursement side of medicine, calling it an "ossified paradigm" that could weigh on cutting-edge therapies like CAR-T cancer therapy..."There are places where I am extremely worried that if we don't adapt the approach to reimbursement soon, we may foreclose therapeutic opportunities,"...The FDA head referenced how radiopharmaceuticals were treated in reimbursement, "underpaying hospitals and forcing them to lose money." Gottlieb warned the same thing is happening now with CAR-T.
- October 26 Pharmacy Week in Review: FDA Addressing Accessibility of Naloxone, Therapy Shows Potential for Treating Pancreatic Cancer (pharmacytimes.com)
Nicole Grassano, PTNN, Pharmacy Week in Review, this weekly video program provides our readers with an in-depth review of the latest news, product approvals, FDA rulings and more.
- CMS eyes Part D catastrophic coverage reforms that would shift risk to insurers (fiercehealthcare.com)
The Trump administration is looking for ways to change the Medicare Part D drug program that would shift more risk to plan sponsors when members reach the final catastrophic coverage stage...The catastrophic coverage tier of Part D kicks in when a member reaches $5,000 in out-of-pocket costs. At that point, patients pay a flat fee or 5% of the negotiated retail drug cost, and the federal government picks up 80% of the remaining costs and plan sponsors pay 15%...That could change. Catastrophic coverage under Part D was initially developed to encourage private insurers to participate, Centers for Medicare & Medicaid Services Administrator Seema Verma said...A lot has changed since then, and now it’s “one example where Part D could be updated or modernized.”...We’re at the point now where it would be better for Part D plans to manage that portion of the benefit,” she said. “That way we could bring competition and negation to that piece as well.”