- In public, lawmakers scold drug distributors. Come campaign season, they accept their cash willingly (statnews.com)
In the run-up to next month’s midterm elections, the country’s three largest distributors alone have given nearly $3 million to congressional campaigns. Key lawmakers from both parties — including many of the ones who publicly shamed the companies for their role in the crisis — have accepted the contributions eagerly...analysis of the current cycle’s campaign finance disclosures, two of the three largest distributors are on pace to exceed their campaign donations from 2016 — a notable increase, since campaign spending tends to stagnate in years without a presidential election...the largest contributions have gone to lawmakers who oversee investigations into those distributors or who play key roles in determining health care and drug policy...From drug companies to insurers, lawmakers routinely accept campaign contributions from the companies across the health care industry that they are tasked with regulating...Sen. Claire McCaskill, who has not accepted campaign cash from distributors, has spoken of the pharmaceutical industry’s ability to sprinkle cash “like fairy dust” around the Capitol — and to use their curried favor to stall legislation that isn’t industry-friendly...
- Why Did I Get the Wrong Rx? (realclearhealth.com)
A recent memo from Centers for Medicare and Medicaid Services clarifies why many Americans aren’t getting the medications they need. The wrong person is choosing your prescription drug, and it isn’t your doctor...starting in 2020, Medicare Part D health plans can implement “indication-based drug therapy.”...Doctors do not treat indications; we treat patients, one at a time, each with his or her own name, unique medical history, and individual reactions to specific medications, whether good or bad...In other words, the person choosing your medications has no medical training, no license to practice medicine, and does not even know your name...Prescribing the wrong Rx for you occurs throughout health care. It is not limited to Medicare...Most health plans require doctors in their panels to use the “fail first” approach, also known as step therapy. When starting treatment, the treating physician can only prescribe the most “cost-effective, medically sound” medication. “Cost-effective” means cheapest drug for the health plan. “Medically sound” means lowest risk of side effects, which often means least likely to be medically effective. After the first drug fails to help the patient, the doctor is then allowed to take the next step with a second drug also chosen by the health plan. Eventually, when all the cheap alternatives fail, the doctor may be allowed to special order the right drug. The bottom line? An insurance actuary, not your doctor, chooses your Rx..
- Trump Signs New Laws Aimed at Drug Costs and Battles Democrats on Medicare (nytimes.com)President Trump Signs Bill to Cut Costs on Prescription Drugs - ENN 2018-10-10 (video) (youtube.com)S.2554 - Patient Right to Know Drug Prices Act (congress.gov)S.2553 - Know the Lowest Price Act of 2018 (congress.gov)
President Trump signed bipartisan legislation...that would free pharmacists to tell consumers when they could actually save money by paying the full cash price for prescription drugs rather than using health insurance with large co-payments, deductibles and other out-of-pocket costs...The legislation on gag clauses has been praised by lawmakers in both parties...The legislation...also includes a provision to combat agreements between drug makers that stifle competition by delaying the marketing of lower-cost copycat versions of expensive biotechnology medicines. Such biologic medicines account for a rapidly growing share of drug spending...Under the new law, manufacturers of the original product and the copy, known as a biosimilar, will have to report such agreements to the Federal Trade Commission, which can challenge them as violations of antitrust laws. The agreements are known as pay-for-delay deals because the branded drug company pays a potential competitor to delay entering the market...
- Nevada again lands at bottom of national health-care ranking (reviewjournal.com)Nevada treading water despite efforts to address doctor shortage (reviewjournal.com)
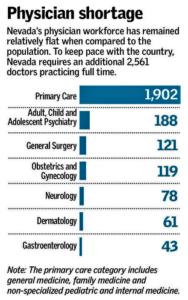
Despite improvements in several areas, Nevada is once again listed at the bottom of a new national health care ranking...Nevada ranked 50th nationwide in a review of more than 100 population-level and patient-level measures published by the Agency for Healthcare Research and Quality. Only the District of Columbia scored lower overall than the Silver State...“There (are) actually areas where Nevada does fairly well — chronic disease care, diabetes, heart failure, stroke...Access to care remains a big problem. Nevada’s physician workforce hasn’t kept up with the state’s ballooning population, causing a doctor shortage...issues in accessing care, including getting an appointment with a primary care physician, having enough time in a doctor’s office and finding a specialist.
- This Week in Managed Care: October 12, 2018 (ajmc.com)
Laura Joszt, Managing Editor at The American Journal of Managed Care. Welcome to This Week in Managed Care from the Managed Markets News Network
- Nevada State Board of Pharmacy – Newsletter – October 2018 (bop.nv.gov)AB 474 (leg.state.nv.us)LCB File No. R047-18 (leg.state.nv.us)
- Assembly Bill 474
- National Pharmacy Compliance News
- FDA Issues Final Guidance Policy on Outsourcing Facilities
- EU-US Mutual Recognition Agreement Now Operational Between FDA and 12 Member States
- US Surgeon General Advisory Urges More Individuals to Carry Naloxone
- Expanding Pharmacists’ Scope of Practice Linked to Improved Cardiovascular Outcomes
- Pharmacists Are Critical to Drug Supply Chain Integrity, States FIP
- Emergency Department Visits for Opioid Overdoses Rose 30%
- Better insurance coverage of non-drug therapies might help ease opioid crisis (reuters.com)Coverage of Nonpharmacologic Treatments for Low Back Pain Among US Public and Private Insurers (jamanetwork.com)
When it comes to non-drug therapies for back pain, U.S. insurance plans vary widely in what they will cover, a new study finds...Private and public insurers are missing important opportunities to promote alternatives to opioids...insurers often provide little or no coverage for evidence-backed interventions for chronic pain such as acupuncture and psychological counseling...“Insurers can be part of the problem or part of the solution,” said study coauthor Dr. Caleb Alexander...at the Center for Drug Safety and Effectiveness...“All too often doctors reach for the quick solution, prescription drugs, especially opioids, to manage pain that would be more effectively and safely treated with non-pharmacological approaches,” Alexander said. “This is a system that is designed with, and fosters, the idea that there is a pill for every ill...
- October 10 Pharmacy Week in Review: Women Pharmacists Day Celebrated, HPV Vaccine Use Expanded (pharmacytimes.com)
Nicole Grassano, PTNN, Pharmacy Week in Review, this weekly video program provides our readers with an in-depth review of the latest news, product approvals, FDA rulings and more.
- UK clinical trials fall as Brexit clouds drug approval process (reuters.com)
The number of new clinical trials started in Britain last year was 25 percent lower than the average for 2009-16, as anxiety about Brexit’s impact on future medicines regulation made companies hesitate about running studies in the country...Drugmakers’ confidence has been dented by fears research data collected in Britain might not be acceptable to the European Medicines Agency after the UK leaves the European Union...The pharmaceuticals industry has long warned that Brexit could have a serious impact on research and access to medicines, unless London and Brussels hammer out a deal for regulatory continuity and close liaison with the EMA...If there is no deal, the UK’s Medicines and Healthcare products Regulatory Agency would have to operate as a stand-alone regulator and there is no clarity over how UK data would be treated by the EMA...
- How Nevada Medicaid struggles with mental health care fraud (reviewjournal.com)
The expansion of Medicaid in Nevada in 2014 made mental health care much more widely available in a state ranked last in the nation for access to such services. It also provided a great opportunity for bad actors...catching those who abuse the Medicaid system is a tortuous process that can either come too late or result in relatively minor penalties...fraudsters are undoubtedly adding to the $56 million deficit Nevada Medicaid predicts it will face in the 2019 fiscal year, up from last year’s $30 million forecast at this time...The Medicaid expansion has certainly “exacerbated” the problem of fraudulent or improper claims in the field of behavioral health...Suspicious claims from mental health providers led Nevada Medicaid to investigate $73 million paid out in the 2018 fiscal year...So far, about $10 million — or 13 percent — has been recovered...