- This billion-dollar dry eye drug is behind Allergan’s controversial patent deal (marketwatch.com)With new bill, Sen. McCaskill looks to end 'brazen' tribal licensing strategy (fiercepharma.com)
Last month, drugmaker Allergan announced that it has made a deal with a New York state American Indian tribe to help protect Restasis from competition, using the tribe’s sovereign immunity as a shield against patent challenges. The deal—the first such move by Allergan and, in the pharmaceutical industry, an unusual one at best—has unleashed a firestorm of criticism, including from lawmakers...Originally, patents on Restasis were set to expire in 2014. But Allergan filed more patents, covering the “specific formulation and the method of using” the product, that expire in 2024...Lawmakers and patient advocates, meanwhile, are concerned not only about the implications for Restasis but whether this will set a pharmaceutical industry precedent...The House Oversight committee wrote to Allergan Chief Executive Brent Saunders on Tuesday asking for documents and information regarding the deal...The agreement “may impair competition across the pharmaceutical industry and ultimately dissuade companies from pursuing less-costly generic alternatives to brand drugs,” according to the letter...Allergan said in a statement that it plans to comply with the information requests...patient advocates say they’re worried...Allergan’s sham patent transfer is an effort to circumvent the law to prevent a cheaper generic of Restasis to come to market,” said David Mitchell, the co-founder and president of the non-profit Patients for Affordable Drugs. “Patients will be hurt by this. Patients are being hurt by this. And it’s an outrage.”
- Specialty Pharmacy Accreditation: To Be or Not to Be, That is the Question (specialtypharmacytimes.com)
Defined in the broadest sense, accreditation means the action of officially recognizing someone as having a particular status or being qualified to perform a particular activity. This definition points to the idea that the act of accreditation provides an individual or organization with an official qualification to perform said duty...The Alphabet Soup of Accreditation...URAC, ACHC, TJC, CPPA: Each of these combinations of letters represent a different accrediting body used by specialty pharmacies. There is not a single authoritative body requesting consistent data reports and patient outcomes that a specialty pharmacy provider (SPP) can utilize. Instead, there is a mix of multiple bodies requesting different kinds and different levels of data...Although the size of the pharmacy and the chosen accrediting body changes the cost for accreditation, it typically costs the pharmacy tens of thousands of dollars each time accreditation is given. And with the growing trend of pharmacies requiring more accreditations, that price is likely to rise...Why is it necessary to have at least 4 major accrediting bodies influencing the behavior of specialty pharmacies?
- Pharmacy Week in Review: October 6, 2017 (pharmacytimes.com)
Nicole Crisano, PTNN. This weekly video program provides our readers with an in-depth review of the latest news, product approvals, FDA rulings and more.
- NCPA-commissioned study: DIR fees could cost CMS $3.4B in next 10 years (drugstorenews.com)
Retroactive pharmacy payment reductions, a portion of direct and indirect remuneration fees, could cost the federal government $3.4 billion between 2018 and 2027. That’s according to a new study from Wakely Consulting...This...study is vitally important in showing that DIR legislation will actually save taxpayers $3.4 billion over 10 years without subtracting any benefits seniors currently receive...For pharmacies, banning these after-the-fact fees is the fair way to achieve predictability in the reimbursement for the medications they buy and dispense...The report evaluates the impact of the Improving Improving Transparency and Accuracy in Medicare Part D Drug Spending Act, which has been introduced in both the Senate and House of Representatives and prohibits retroactive pharmacy payment reductions as claims without any defect, impropriety or fraud in Medicare Part D...The legislation is part of NCPA’s efforts to end DIR Fees, which make up a small amount of overall DIR within Medicare Part D, the majority of which is made up of manufacturer rebates
- New Jersey sues Insys as opioid maker settles with Massachusetts (reuters.com)
New Jersey...accused Insys Therapeutics Inc of engaging in a fraudulent scheme to boost sales of a fentanyl-based cancer pain drug, as Massachusetts announced a $500,000 settlement with the drugmaker to resolve similar allegations...The lawsuit by New Jersey Attorney General Christopher Porrino accused Insys of illegally directing its sales force to push prescriptions of Subsys for a broader range of patients than the opioid drug was approved for, and at higher doses...The lawsuit...alleged Insys also paid kickbacks, including sham speaker fees to medical practitioners to prescribe Subsys and defrauded insurers into paying for it...The lawsuit said Insys’ greed put hundreds of lives in jeopardy and led to the 2016 overdose death of a New Jersey woman who was prescribed Subsys to treat fibromyalgia.
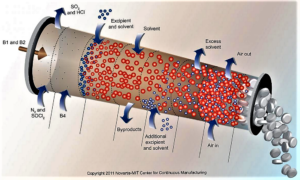
- Continuous Manufacturing: Pfizer, Vertex, AstraZeneca and Others Weigh FDA Plans (raps.org)
The US Food and Drug Administration has been encouraging the adoption of continuous manufacturing techniques...and several companies recently offered the agency some suggestions to refine its work around the developing technology...continuous manufacturing allows companies to move more seamlessly and efficiently...Last week, FDA finalized guidance on how manufacturers can participate in the agency’s program to advance continuous manufacturing...And in a blog post, Michael Kopcha, director of FDA's Office of Pharmaceutical Quality, pointed to Vertex's cystic fibrosis drug Orkambi (lumacaftor/ivacaftor) and Janssen's HIV treatment Prezista (darunavir) as examples of companies successfully using continuous manufacturing after engaging with FDA's emerging technology team...Vertex Pharmaceuticals...noted several contradictions in how batch size is described in an FDA document and sought further clarity and certainty regarding FDA’s understanding and expectations regarding batch size...AstraZeneca...asked if FDA might consider harmonizing the assessment process of the changes relating to continuous manufacturing, including a mechanism by which there could be some mutual recognition across countries participating in the International Council on Harmonization. AstraZeneca also said it "does not see the need" for a full ICH guideline on continuous manufacturing, which the company says FDA has been supporting. But the European drug industry group known as EFPIA is suggesting a Q&A document based on ICH Q8 and AstraZeneca says it "concurs with that approach."
- Nevada explores options as Children’s Health Insurance Program expires (reviewjournal.com)
Nevada officials are exploring alternative avenues for insuring more than 26,300 children in the state covered under the Children’s Health Insurance Program if Congress doesn’t reauthorize the program, which is set to expire Saturday...Congress is expected to reauthorize the CHIP program through a bipartisan bill, though that could be weeks away. And with the turmoil in Congress lately, state officials are taking no chances...The Department of Health Care Financing and Policy is working with state partners to identify alternative sources of funding for the program if it is not reauthorized, deputy administrator Cody Phinney said ...“We would have to find other funding sources and we’d have to look at our options for limiting the services that are available, but our first role is to maintain those services,” Phinney said...the federal government pays nearly the entire annual $43 million cost of the program in Nevada...The state has ‘reserve funding’ to operate the health-care program for the next few months. However if Congress does not quickly reauthorize CHIP, states like Nevada will need to either send notices of termination to program beneficiaries or develop alternative funding...
- Las Vegas Strip shooter prescribed anti-anxiety drug in June (reviewjournal.com)Drug given to Paddock calms some, provokes others, experts say (reviewjournal.com)
Stephen Paddock, who killed at least 58 people and wounded hundreds more in Las Vegas...with high-powered rifles, was prescribed an anti-anxiety drug in June that can lead to aggressive behavior...Records from the Nevada Prescription Monitoring Program...show Paddock was prescribed 50 10-milligram diazepam tablets by Henderson physician Dr. Steven Winkler on June 21...Diazepam...studies have shown can trigger aggressive behavior. Chronic use or abuse of sedatives...can also trigger psychotic experiences...“If somebody has an underlying aggression problem and you sedate them with that drug, they can become aggressive,” said Dr. Mel Pohl, chief medical officer of the Las Vegas Recovery Center. “It can disinhibit an underlying emotional state. … It is much like what happens when you give alcohol to some people … they become aggressive instead of going to sleep.”
- This Week in Managed Care: October 6, 2017 (ajmc.com)
Laura Joszt, assistant managing editor at The American Journal of Managed Care. Welcome to This Week in Managed Care from the Managed Markets News Network
- Express Scripts: Specialty meds driving up US drug spend (biopharmadive.com)
An estimated three out of every 1,000 Americans ring up a bill of more than $50,000 in annual prescription drug costs last year, according to a new analysis of health plan members published...by Express Scripts... The number of people who meet this threshold for high pharmaceutical expenditures has risen sharply, by 35%, since the PBM's last report on the trend in 2014. While numerically small, this group of patients accounted for more than 20% of total U.S. spending on prescription drugs in 2016...higher utilization of pricey specialty medicines for cancer, multiple sclerosis and rare diseases was the primary driver of spending among patients with annual pharmacy costs over $50,000. Yet that was a change from 2014, when new hepatitis C drugs and compounded medicines goosed spending...Nearly 96% of the plan members who cleared the $50,000 in annual spending threshold used specialty medicines, most notably cancer therapeutics. While the average annual cost of oncology drugs was lower than some other specialty categories, a quarter of all spending by this group was on cancer treatments...