- This Week in Managed Care: June 23, 2017 (ajmc.com)
Laura Joszt, assistant managing editor at The American Journal of Managed Care. Welcome to This Week in Managed Care from the Managed Markets News Network
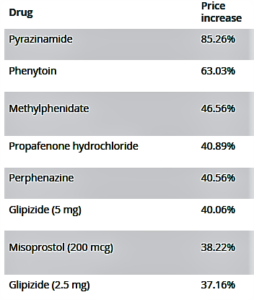
- Why did these generic drugs’ prices jump as much as 85%? (marketwatch.com)
On June 13, as members of a Senate health panel gathered to discuss the rising cost of prescription drugs, the prices of 14 common medications were increased by some 20% to 85%...The blame for rising drug prices once fell squarely on drug makers. But it has shifted at least in part to industry middlemen, with critics saying those companies benefit from high prices and help drive them up. In turn, the middlemen point back to drugmakers, charging that they set the prices in the first place...The corporate blame game can make it hard to determine who is actually benefiting from higher drug prices. June 13’s price increases are a case in point as to why this has become a harder question to answer than it might at first seem...When it comes to drug pricing, AmerisourceBergen is best known as a bellwether for industry trends...competitors including McKesson and Cardinal Health make money based on drug sales and can thus predict how much prices will rise or fall in a given year. And, if they negotiate prices with a pharmacy, they can also play a role in setting prices...when questioned about these increases, executives from drug manufacturers...have pointed instead to pharmaceutical middlemen, which benefit from higher prices, too...But the role of these industry players, including pharmacy-benefit managers...may be shifting out of the regulatory limelight.
- FDA moves to prevent Pharma from ‘gaming’ generic drug system (reuters.com)
The...Food and Drug Administration moved...to prevent pharmaceutical companies from "gaming" the system to block or delay entry of generic rivals…FDA Commissioner Scott Gottlieb said...that the agency plans to hold a public meeting...to identify ways pharmaceutical companies are using FDA rules to place obstacles in the way of generic competition..."We know that sometimes our regulatory rules might be 'gamed' in ways that may delay generic drug approvals beyond the time frame the law intended, in order to reduce competition,"..."We are actively looking at ways our rules are being used and, in some cases, misused."...These obstacles can include limiting the availability of branded products for testing by generic companies, or prolonging negotiations with generic companies over the implementation of shared risk-management programs...
- AMA calls for more transparent prescription costs (healio.com)
In response to the recent spike of many prescription drug prices, the AMA adopted several policies to provide patients with more information about the drugs that they are prescribed and a rationale for price increases…Taken together, these policies would bring much needed transparency to drug pricing and provide a clear benefit to consumers struggling with exorbitant costs…There seems to be no logic — or warning — to these price spikes…The AMA urged federal agencies to require that manufacturers list the suggested retail prices of medications on direct-to-consumer ads...In addition, AMA encouraged drug companies to notify the public of price increases of more than 10% for certain medications over a 12-month period...
- Week in Review: June 23 (pharmacytimes.com)
Kaitlyn Ellie, PTNN. This weekly video program provides our readers with an in-depth review of the latest news, product approvals, FDA rulings and more.
- Working Smarter: Establishing an Effective Serialization Architecture (pharmtech.com)Serialization and the Drug Quality & Security Act (pharmamanufacturing.com)
The upcoming serialization requirements in the European Union and the United States have presented pharmaceutical companies with the challenge of balancing data integrity with performance when designing the appropriate information architecture...The pharma sector is currently undergoing the process of introducing new systems and processes for serialization...Companies offering networks for the storing and sharing of vast amounts of serialization data are challenged with creating a shareable world that is also scalable. For pharmaceutical companies, serialization will require a paradigm shift in IT architecture to deal with the combination of the vast amount of data stored within network databases and the operational processes associated with the upcoming requirements...In an industry as highly regulated and safety critical as the pharmaceutical sector, the integrity of the real world must meet the volume and performance of the virtual world. Cloud networks for serialization must offer security, together with speed and scalability especially with the introduction of new drug traceability requirements across the globe...
- EU court: Vaccines can be blamed for illnesses without proof (ktvn.com)
The highest court of the European Union ruled…that courts can consider whether a vaccination led to someone developing an illness even when there is no scientific proof…The decision was issued…in relation to the case of a Frenchman known as Mr. J.W., who was immunized against hepatitis B in late 1998-99. About a year later, Mr. J.W. was diagnosed with multiple sclerosis. In 2006, he and his family sued vaccine-maker Sanofi Pasteur in an attempt to be compensated for the damage they claim he suffered due to the vaccine. Mr. J.W. died in 2011… the EU's top court said that despite the lack of scientific consensus on the issue, a vaccine could be considered defective if there was "specific and consistent evidence," including the time between a vaccine's administration and the onset of a disease, an individual's previous state of health, the lack of any family history of the disease and a significant number of reported cases of the disease occurring following vaccination.
- Mylan board survives ouster attempt, but shareholders reject rich pay packages (statnews.com)
Mylan stockholders voted to reelect its board at the annual meeting...rebuffing an unusual and highly public campaign from some top shareholders determined to oust many of the directors, including the CEO...But the company also suffered a rebuke as its shareholders voted against a measure to approve executive compensation. That vote doesn’t force Mylan to reduce its pay packages, but most companies do try to be responsive to such votes. Mylan issued a statement saying it would take the shareholder views into account in designing future compensation packages...The fact that the vote over executive compensation failed is unusual for a company of this size...Usually companies respond by making reforms and we certainly hope Mylan will listen to shareholders and discontinue excessive pay, but they seem to shrug off even the most well-founded criticism…
- Drugmaker Mylan gets boost from unlikely source: coal (reuters.com)
Mylan N.V. is best known for producing EpiPen emergency allergy treatments and generic drugs...But a non-pharmaceutical offering – refined coal – has quietly generated hundreds of millions of dollars of tax credits for the company over the last six years that have boosted its bottom line...Since 2011, Mylan has bought 99 percent stakes in five companies across the U.S. that own plants which process coal to reduce smog-causing emissions. It then sells the coal at a loss to power plants to generate the real benefit for the drug company: credits that allow Mylan to lower its own tax bill...Mylan is one of only a few public companies, and the only publicly-traded pharmaceutical maker, that uses these tax credits...
- Will CVS Health’s Point-of-Sale Rebates Deflate the Gross-to-Net Bubble—and Disrupt the PBM Business? (drugchannels.net)
I examined the magnitude of the gross-to-net bubble—the growing spread between a manufacturer’s list price for a drug and the net price to a third-party payer after rebates...The bubble directly affects patients’ out-of-pocket costs. Many patients now have benefit plans with deductibles and are therefore required to pay the full, undiscounted cost of their prescriptions. Patients taking specialty drugs face large coinsurance computed using the undiscounted list price...One solution replaces formulary payments made to plan sponsors with prescription discounts for patients at the point of sale. Last week, CVS Health became the first pharmacy benefit manager to publicly embrace and explain this alternative benefit design...Do point-of-sale rebates solve the patients’ problems that the gross-to-net bubble causes? And will this benefit design mark the beginning of the end for the PBMs’ traditional economic model?