- Gilead snaps up Sarepta’s priority review voucher for $125M (biopharmadive.com)
Hoping to speed up future regulatory review for its drug candidates, Gilead has agreed to buy a priority review voucher from Sarepta Therapeutics for $125 million...Sarepta had obtained the voucher — a transferrable credit designed to speed review by the Food and Drug Administration by four months — for winning approval of its disease-modifying treatment for Duchenne muscular dystrophy last year...Sale of the voucher, albeit for a lower price than some had expected, will bolster Sarepta's cash position and help fund clinical development of Sarepta's pipeline and manufacturing scale-up…For Gilead, the voucher could be used to speed review for one of its several late-stage candidates. The $125 million is a relative bargain as well, compared to both the recent prices paid by Sanofi and AbbVie as well as to Gilead's large cash hoard.
- A Call For The FDA To Raise The Bar For Clinical Trials Is Flawed (forbes.com)
As the new Trump administration begins to take shape, there are concerns that new leadership at the FDA will call for less bureaucracy and red tape, thereby lowering the bar for new drug approvals. The view is that onerous regulations are preventing life-saving medications from getting to those who most need them. Lowering the standards for drug approvals may indeed allow for earlier patient access to drugs but...liberalization of current regulations would be a mistake. Such actions will unleash drugs that will ultimately prove to be ineffective and, in some cases, harmful rather than beneficial...the specter of deregulation, comes a call to increase the requirements for allowing early clinical trials of exploratory new medicines...Trials of ineffective therapies place burdens on society...Drug development soaks up financial and research resources...expenses wasted on ineffective therapies are often passed on to healthcare systems in the form of higher drug prices. The biopharmaceutical industry is testing “duds” and wasting precious resources because of unreasonable hope for a major commercial payoff...The biopharmaceutical industry is already heavily regulated. Current standards shouldn’t be lowered...
- Genentech lobbyist’s life and death makes pharma waves (fiercepharma.com)
A Genentech lobbyist who generated enormous sales for the company allegedly kept millions in consulting payments for himself and ended his own life after authorities and the company began looking into the charges...During his time lobbying for Roche and its Genentech unit, Evan Morris’ tactics boosted the company's top line by hundreds of millions of dollars, with the company's flu drug Tamiflu and cancer treatment Avastin among the products that benefited...Under investigation for embezzlement in July 2015, Morris committed suicide at a Virginia golf course...Morris’ lavish life, ...featured expensive houses, wines, influential contacts and more, before it came quickly crashing down. An obituary for Morris simply says he “resided in Alexandria, VA.” He was born in 1977 and died on July 9, 2015, the obituary says.
- This Week in Managed Care: February 17, 2017 (ajmc.com)
Laura Joszt, assistant managing editor at The American Journal of Managed Care. Welcome to This Week in Managed Care from the Managed Markets News Network
- Pharmacy Week in Review: February 24, 2017 (pharmacytimes.com)
Brian Haug, President of Pharmacy and Managed Markets, Pharmacy Times (PTNN) This weekly video program highlights the latest in pharmacy news, product news, and more.
- How insurance reimbursement affects Nevada health care (reviewjournal.com)
It’s been in the air for much of the past year, and as many of the some-feared and some-promised changes have happened around us, those health care business owners who rely on insurance reimbursement have waited with bated breath for a sign of what’s to come. The Trump administration has promised, via stump speech and now executive order, the rapid repeal and replacement of the Affordable Care Act, but what is simple to say is often far more difficult to accomplish.
- MEDICARE UNSUSTAINABILITY... the U.S. population continues to age... This has contributed to explosive growth in Medicare participation...
- INSURING THE UNINSURED...the American public has determined to no longer accept 30 million uninsured Americans who are not Medicare-eligible as the status quo. Caring for these individuals through catastrophic care via public emergency rooms has become untenable both fiscally and morally…
- VALUE-BASED CARE...care reimbursement models have been established to replace the traditional fee-for-service model that has dominated American health care for generations. FFS models reimburse health care providers for services rendered in the form of treatment or testing and have seen unsustainable inflation over the past 10 years…
- ELECTRONIC HEALTH RECORDS...One of the key elements of a VBC system is the interoperability of health care records, which permits and encourages (by ease of use) coordination of care across providers...This reduces redundancies and the probability of contraindicated treatment being administered in good faith…
- ACCOUNTABLE CARE ORGANIZATIONS...are groups of health care providers who come together to voluntarily give coordinated high-quality care to their Medicare patients. ACOs tie payments to quality metrics and the cost of care…
- WHAT’S NEXT?...Increase capacity utilization...Consolidation…
- SCALING UP...While apparently antithetical to the current market, scaling up is the external version of increasing capacity utilization. Often a practice’s assets can only be maximized by increasing the scale of the practice...
- Pharma lobby launches crusade against Cuomo’s ‘flawed’ drug pricing plan in NY (fiercepharma.com)
Pharma has heard enough of New York Governor Andrew Cuomo’s ideas for lowering drug prices. Just a month after the governor unveiled his plan, the industry’s trade group is rolling out a counteroffensive urging state officials to “Prescribe Real Solutions”...Gov. Cuomo’s plan would create a board to rule on “fair prices” for certain expensive drugs. Then, the state would mandate that Medicaid refuse to pay more than that for those meds...Cuomo's proposal also factors into private market sales. If a pharma company sold into New York at a higher price than the board’s "fair price," the state would collect a surcharge...PhRMA is having none of that. The group’s Prescribe Real Solutions website asks the public to “demand real solutions” from their lawmakers...PhRMA’s deputy vice president for state advocacy in New York, maintains that Cuomo's proposal "does nothing to improve patient access to medicines, bring life-saving drugs to the market or create jobs" in the state..."This is not the time for unworkable proposals that would create new bureaucracies without actually addressing any of the factors that impact the prices paid by patients,"...
- Trump is promising big changes at the FDA — here’s how drugs are approved today (businessinsider.com)
At least one of President Trump's possible picks to head the Food and Drug Administration has a radical idea for when drugs should come to market...Jim O'Neill, managing director at Mithril Capital, has said that he is in favor of approving drugs that are proven to be safe, even before they're shown to be actually effective...Regardless of who Trump picks in the end, his interest in cutting regulation at the FDA is clear..."We're going to be cutting regulations at a level that nobody's ever seen before," Trump said in a meeting with pharma executives...As it exists right now, the FDA approval process can be a long and expensive…
- Cheaper drugs from Canada? Pharma despises the idea, but top senators are pushing HHS chief to try it (fiercepharma.com)
Instead of being gouged on the prices for old drugs, Americans could import certain meds from Canada if a bipartisan group of senators get their way...Sens. Klobuchar, Chuck Grassley, and John McCain...are pushing President Donald Trump’s new Department of Health and Human Services Secretary, Tom Price, to authorize cheap drug imports under strict circumstances...Their bill, the Safe and Affordable Drugs from Canada Act, would require the FDA to set up a “personal importation program” to allow individuals to import 90-day supplies of their meds from Canadian pharmacies...To qualify for importation, the senators' proposal would require products to be off patent or no longer marketed in the U.S. by the original developer. They'd need to be free of direct competition and to have seen a “significant, unexplained” price hike. The imported product would also need to be produced by a reputable company. The bill additionally calls for fast-track FDA reviews of competing drugs...Imported drugs wouldn’t “be subject to the U.S. Food and Drug Administration’s robust safety requirements, and there would be no way to trace the country of origin for the imported products...
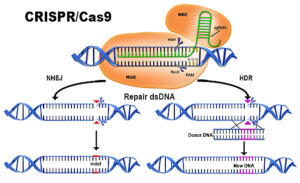
- Broad Institute notches win in CRISPR patent battle (biopharmadive.com)
In a hotly anticipated judgment, the U.S. patent office...ruled that key patents held by the Broad Institute of MIT and Harvard on the gene-editing technology CRISPR-Cas9 do not overlap with competing claims from the University of California...UC may now receive a patent covering broader claims on the revolutionary tech...the Patent Trial and Appeal Board ruled the claims of UC and the Broad to be patentably distinct subject matter, leading the three judges to declare a judgment of non-interference...Put into layman's terms, the claims of the UC and the Broad are distinct enough so as to be separately patentable and therefore don't overlap with each other. This effectively supports the Broad's existing patents, while sending the UC's pending patent application back to the initial patent examiner...UC with a patent on use of CRISPR in all cells and the Broad with a patent for use of CRISPR specifically in eukaryotic cells...If that were to happen, biotechs operating in the space could end up having to license the tech from both UC and the Broad.