- NCPA stands with NY patients, pharmacists after Cuomo veto (chaindrugreview.com)AARP praises Governor Cuomo’s plan to tackle high Rx drug costs (chaindrugreview.com)
Despite aggressive advocacy efforts by state-based pharmacy organizations and individual New York pharmacists, Gov. Andrew Cuomo this week vetoed legislation to help to rein in costly pharmacy benefit manager practices by giving the superintendent of insurance licensing and regulatory authority over PBMs. This regulatory authority would put an end to the lack of transparency, oversight, and accountability that has allowed PBMs to engage in anticompetitive practices to the harm of the state’s patients and small-business community pharmacies...READ MORE
- $3K for folic acid? CVS Caremark takes aim at ‘hyperinflated’ drug prices (fiercehealthcare.com)
CVS Caremark is saving money on drug costs by kicking specific products with high inflation off their formularies...The pharmacy benefit manager launched its program for “hyperinflation” drug removals in 2017 in which it will take drugs off its template formulary if they have far cheaper equivalents and their high prices aren’t backed by quality metrics...So far, they've identified five drugs to remove as the default option for docs...Through these efforts, Caremark has saved its PBM clients an average of $15 per 30-day supply on drugs—clients on this formulary model paid on average $88.30 for a 30-day drug supply, compared to $102.58 for other formulary designs...As the program is focused on products like that with high costs compared to alternatives, just five have been pulled from formularies so far—leading to a 99% drop in member use...READ MORE
- Lawmakers hear bill to ban rules barring pharmacists from telling patients about less expensive, generic drugs (thenevadaindependent.com)
The legislation, which GOP Assembly members Melissa Hardy and Glen Leavitt presented to the Assembly Commerce and Labor Committee on Monday, would bar pharmacy benefit managers, or PBMs, from stopping a pharmacist from telling patients about the availability of a less expensive, generic or more effective drug, or a less expensive manner of purchasing a drug. The proposal builds upon a pharmacy gag ban passed by the Legislature in 2017 that prevented PBMs from blocking pharmacists from sharing information about the copay or coinsurance for a prescription drug or the clinical efficacy of a less expensive alternative drug...READ MORE
- How Mergers Will Affect Pharmacists (drugtopics.com)
The Cigna-Express Scripts merger has gotten a go-ahead from the Department of Justice, but DOJ has not ruled on the CVS-Aetna merger at press time...Both deals have shareholder backing... I think it’s part of an overall trend...Effects on Pharmacists...Frederick S. Mayer...CEO of Pharmacists Planning Services Inc...fears that they could result in loss of pharmacy jobs due to closures of independent pharmacies that can no longer compete. Chain pharmacists could also have less job security as locations may close. Mayer also says consolidation could lead to higher prices, lower quality, and less choice for consumers...Pharmacists...trained eight years for their PharmD, and now they are counting, pouring, and typing due to mergers,” says Mayer, who adds that pharmacists in larger settings don’t have adequate time for patient counseling...Over the past 10 years, mergers have resulted in poorer choices of medication for consumers and patients...Chains that are in one of these vertically integrated systems have guaranteed volume without competition on price...Perry Cohen, CEO of The Pharmacy Group...Companies responding to the need for new care models for healthcare services. The marketplace needs new care models and wants to embrace these companies that get ahead of the curve...More Mergers Coming... more vertical mergers and acquisitions...The horizontal is being driven a lot by the reimbursement pressure...The vertical is much more strategic around the control of the overall person’s healthcare...
- Has Physician Specialty Dispensing Peaked—And Should They Blame PBMs? Everyone wants to be a specialty pharmacy—but it’s getting harder to compete. (drugchannels.net)
Consider the boom in pharmacies operated by physician practices. The growth in oral and patient self-injectable specialty drugs has encouraged physicians to dispense these products from their offices and clinics. For example, almost half of all oncology practices now dispense specialty drugs to their patients...the share of oncology practices dispensing prescriptions has declined for the first time in at least six years. I suspect that we are at a turning point in the growth of physician practice dispensing...this development reflects how PBMs and their plan sponsor clients are managing specialty channels...PBMs offer financial carrots that entice plan sponsor to shift prescriptions into PBM-owned specialty pharmacies. This dynamic creates novel competitive conflicts between historically separate drug channel participants. Meanwhile, physicians are learning the perils of competing with vertically-integrated channel organizations...READ MORE
- White House pulls drug rebate rule to relief of payers (biopharmadive.com)In win for pharma, Trump TV drug price rule struck down (biopharmadive.com)
The White House will withdraw a controversial plan to ban drugmaker rebates to pharmacy benefit managers in Medicare and Medicaid, stepping back from what the administration had once billed as "the most significant change in how Americans' drugs are priced at the pharmacy counter."..."Based on careful analysis and thorough consideration, the President has decided to withdraw the rebate rule...noting ongoing discussions about potential legislation around drug pricing...Drugmakers had supported the proposed rule, which fit with pharma's public relations campaign attacking the role played by PBMs in keeping drug costs high...READ MORE
- Nevada State Board of Pharmacy News (bop.nv.gov)
Board Members
Leo Basch, PharmD, RPh, Las Vegas
Robert Sullivan, Reno
Jason Penrod, PharmD, RPh, Reno
Kevin Desmond, RPh, Reno
Wayne Mitchell, PharmD, RPh, Carson City
Melissa Shake, PharmD, RPh, Las Vegas
Jade Jacobo, PharmD, JD, RPh, Las Vegas
Retirement of the Executive Secretary
- Larry L. Pinson, PharmD, RPhNew Reno Office -
985 Damonte Ranch Parkway, Suite 206, Reno, NV 89521.
Board Member UpdateNevada Medicaid Initiates Antibiotics Prior Authorization Criteria - Nevada Department of Health and Human Services
National Pharmacy Compliance NewsFinal Guidance Documents Address FDA Policies Related to DSCSA
First FDA-Approved Drug Containing Extract From Cannabis Plant to Be Placed in Schedule V
ASHP Guidelines Provide Recommendations for Preventing Patient Harm From Medication Errors
FDA’s Final Guidance Documents Address Compounding and Repackaging of Radiopharmaceuticals
Pharmacy Toolkit Encourages Conversations With Patients About Prescription Opioids
Biosimilars Added to FIP’s Policy on Pharmacists’ Right to Substitute a Medication
FDA Offers CE Course on Reducing Hypoglycemic Events in Patients With Type 2 Diabetes - Leveraging Health Literacy and Patient Preferences to Reduce Hypoglycemic Events in Patients with Type 2 Diabetes
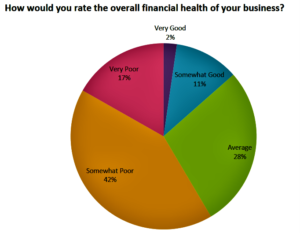
- Study: Local pharmacies pushed to brink by pharmacy benefit “monopolies” (chaindrugreview.com)NCPA SURVEY: Health of Independent Pharmacy (ncpa.co)
A substantial majority of independent pharmacies say they may close their doors in the next two years, and the main culprits are multi-billion-dollar corporate middlemen who are shaking them down for fees on medicines long after the point of sale, according to a new survey by the National Community Pharmacists Association...“Neighborhood pharmacies are being mugged in broad daylight and no one in Washington is doing anything about it,” said NCPA CEO B. Douglas Hoey. “If Congress or the administration don’t act soon, we’re going to see a wave of layoffs and store closures that will leave many patients stranded without access to a local pharmacist.”...READ MORE
- Not So Fast on Ending Rebates for Prescription Drugs (realclearhealth.com)
Give President Trump credit for acting on his promise to bring down prices for prescription drugs. But one policy idea his administration has proposed needs a second look...The Department of Health and Human Services has proposed a rule that would end rebates that drug companies pay to Part D and Medicaid-managed organizations for the prescription drug equivalent of preferential shelf placement and instead require savings from any such rebates be passed along to consumers... if this regulation goes final...it may even mean lower prices for some drugs in some cases...But Big Pharma...will realize a windfall of up $100 billion per year...what Part D participants pay in premiums and taxpayers shell out for Medicare and Medicaid – would go up...READ MORE
- CVS offers ‘guaranteed net cost’ for pharmacy benefit clients (reuters.com)
Pharmacy chain and benefits manager CVS Health Corp...said...it will offer a new prescription benefit option guaranteeing its health plan clients 100 percent of any rebates, discounts or other fees paid by drugmakers...The new plan model is aimed at providing greater drug cost simplicity, predictability and transparency...Under its new option, CVS takes on the risk of drug price inflation and shifts in drug use - at least for the term of each contract...The new model guarantees average spending per prescription across each distribution channel – retail, mail order and specialty pharmacy...