- Express Scripts: Specialty meds driving up US drug spend (biopharmadive.com)
An estimated three out of every 1,000 Americans ring up a bill of more than $50,000 in annual prescription drug costs last year, according to a new analysis of health plan members published...by Express Scripts... The number of people who meet this threshold for high pharmaceutical expenditures has risen sharply, by 35%, since the PBM's last report on the trend in 2014. While numerically small, this group of patients accounted for more than 20% of total U.S. spending on prescription drugs in 2016...higher utilization of pricey specialty medicines for cancer, multiple sclerosis and rare diseases was the primary driver of spending among patients with annual pharmacy costs over $50,000. Yet that was a change from 2014, when new hepatitis C drugs and compounded medicines goosed spending...Nearly 96% of the plan members who cleared the $50,000 in annual spending threshold used specialty medicines, most notably cancer therapeutics. While the average annual cost of oncology drugs was lower than some other specialty categories, a quarter of all spending by this group was on cancer treatments...
- Wal-Mart, Walgreens, CVS turn up the heat on generic drugmaker deals (reuters.com)
The largest U.S. retail pharmacies, including Wal-Mart Stores Inc and Walgreens Boots Alliance Inc, are wielding more leverage when buying generic drugs, accelerating a decline in prices likely to affect drug companies for some time...That pressure is exacerbated by efforts from U.S. health regulators to speed approval of copycat drugs...The extent of the shift became clearer this week, when wholesale drug distributors Cardinal Health Inc and AmerisourceBergen Corp, as well as top global generic drugmaker Teva Pharmaceutical Industries Ltd, warned of generic price declines of as much as 9 percent through the end of the year…Walgreens formed a drug-buying partnership with AmerisourceBergen in 2013, and earlier this year partnered with pharmacy benefit manager Express Scripts Holdings Co. Retailer CVS Health Corp has tied up with Cardinal Health and, more recently, Wal-Mart has joined with McKesson Corp to source generic drugs. Industry analysts said the alliances took some time to become effective, but their power over negotiations is becoming clear.
- New Pain Drug Likely To Face Price Challenges From Payers (forbes.com)
Centrexion Therapeutics announcing six-month data with its drug, CNTX-4975, for the treatment of moderate to severe knee osteoarthritis pain. The results are from a Phase 2b trial...and Centrexion is pretty excited by what has been seen so far:..The new data show large and statistically significant pain relief...a single 1 mg injection...resulted in large levels of pain reduction compared to baseline and statistical separation from placebo...These data represent the largest reductions seen in knee osteoarthritis reported for any drug treatment, marketed or in development…the active component is capsaicin...CNTX-4975 is "based on Centrexion’s proprietary STRATI technology (Synthetic TRans cApsaicin ultra-pure Injection), a highly potent, ultrapure, synthetic form of trans-capsaicin."...In certain ways, CNTX-4975 is reminiscent of the EpiPen. The active component of the latter is epinephrine, which, like capsaicin, is a drug that’s been known for decades. It’s the injector device, however, and not the drug, that drives Mylan’s proprietary position–and price–for the EpiPen. Similarly, the STRATI technology is what protects CNTX-4975 competitively, as anyone can easily access trans-capsaicin. In addition, epinephrine and trans-capsaicin are cheap drugs. These aren’t complex biologic molecules...The major cost will be for the STRATI technology...it is possible that Centrexion and its investors are going to demand premium pricing for the unprecedented pain relief...How will payers react?
- Inside the ‘Scorpion Room’ Where Drug Price Secrets Are Guarded (bloomberg.com)
PBMs occupy a key crossroads of the health system, acting as a nexus among insurers, employers and drug companies. Through a complex web of agreements they help decide what drugs are covered by a patient’s insurance, and how much they’ll cost at the pharmacy counter. The problem, say critics, is that opacity makes it hard for employers to know how much the PBM is paying and profiting on each transaction -- an impression reinforced by restrictions on who can audit them and how.
- Swelling Costs - President Donald Trump has repeatedly complained about high drug prices
- Wrangling Rebates - The most carefully guarded secrets of the PBM industry involve tens of billions of dollars in rebates they collect from drug companies. Those payments help drugmakers secure favorable spots on medication menus that PBMs offer to millions of patients.
- Other Avenues - Rebates are only one way drugmakers pass money to PBMs. Others include fees for care management, administration and inventory procurement.
- Will Amazon really get into drug sales? It’s in talks with PBMs already, report says (fiercepharma.com)
Rumors that Amazon is looking to parachute into the drug field are getting louder. Amazon is already in talks with pharmacy benefits managers...and that poses a larger threat to the pharma industry than some might realize...The retail giant has stayed quiet about its pharma ambitions... a report saying the category-killer is in talks with mid-size PBMs "in an effort to get into various contract arrangements,"...A potential entrance into the drug business could take 18 to 24 months...but Amazon could be a "bigger threat" to the pharmaceutical status quo than many appreciate...There's plenty of reason Amazon might want to get into the drug supply chain...the field is worth $125 billion each year, or 30% of U.S. net pharma spending. To start, the company might offer a strong user experience and a top-notch logistics network, later looking to change transparency dynamics on pricing...the company might partner with a PBM as a "path of least resistance." Other routes into pharma for Amazon would be as an online pharmacy, a retail plus online pharmacy, an integrated PBM or a distribution player to pharmacies...
- CVS Health removes 17 drugs from formulary, adds outcomes-based program (biopharmadive.com)
CVS Health...put out its standard control formulary for 2018, days after competitor Express Scripts announced its own drug coverage list for next year...Last year, CVS made biosimilars preferable over their reference product on its formulary, while this year the PBM expects to expand value-based deals to add further benefit for its customers...last year...it opted to include the highly touted, but still very new class of biosimilar products over longer-used reference products...This year, CVS Health looks set to change the game once again with an outcomes-based management program that will specifically target drugs for breast cancer, non-small cell lung cancer, obesity and chronic obstructive pulmonary disease...In each of these cases, manufacturers will have to cover costs over a pre-specified threshold if patients don't reach certain outcomes...Outcomes-based strategies have long been talked about as a means to control drug pricing. But there have only been a handful of such agreements put into practice and usually with specific drugmakers for specific products...CVS Health will remove 17 drugs from the 2018 formulary list across 10 drug classes...
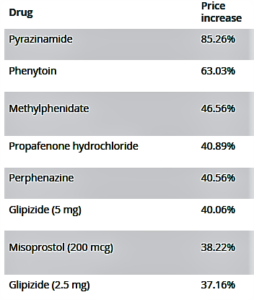
- Why did these generic drugs’ prices jump as much as 85%? (marketwatch.com)
On June 13, as members of a Senate health panel gathered to discuss the rising cost of prescription drugs, the prices of 14 common medications were increased by some 20% to 85%...The blame for rising drug prices once fell squarely on drug makers. But it has shifted at least in part to industry middlemen, with critics saying those companies benefit from high prices and help drive them up. In turn, the middlemen point back to drugmakers, charging that they set the prices in the first place...The corporate blame game can make it hard to determine who is actually benefiting from higher drug prices. June 13’s price increases are a case in point as to why this has become a harder question to answer than it might at first seem...When it comes to drug pricing, AmerisourceBergen is best known as a bellwether for industry trends...competitors including McKesson and Cardinal Health make money based on drug sales and can thus predict how much prices will rise or fall in a given year. And, if they negotiate prices with a pharmacy, they can also play a role in setting prices...when questioned about these increases, executives from drug manufacturers...have pointed instead to pharmaceutical middlemen, which benefit from higher prices, too...But the role of these industry players, including pharmacy-benefit managers...may be shifting out of the regulatory limelight.
- CVS Health Is Sued Over ‘Clawbacks’ of Prescription Drug Co-Pays (bloomberg.com)
CVS Health Corp. and Walgreens Boots Alliance Inc. were sued by California customers who accused the drugstore operators of charging co-payments for certain prescription drugs that exceed the cost of medicines...CVS...overbilled consumers who used insurance to pay for some generic drugs and wrongfully hid the fact that the medicines’ cash price was cheaper...Walgreens...used the same clawback tactic...The lawsuits follow at least 16 other cases...targeting drugstore chains’ alleged co-pay clawback practices. The clawback occurs when patients hand over co-payments set by a pharmacy benefit manager that exceed the actual cash cost of the drug. The benefit managers pocket the difference…Most patients never realize there’s a cheaper cash price because of clauses in contracts between pharmacies and benefit managers that bar the drugstore from telling people there’s a lower-cost way to pay...Schultz (Megan Schultz v. CVS Health Corporation, 17-cv-359, U.S. District Court for the District of Rhode Island)...contends that CVS’s clawback agreements with benefit managers such as Express Scripts, CVS Caremark and OptumRx violate federal racketeering and insurance laws and works to artificially inflate prescription costs...
- Express Scripts shuts out 64 branded drugs from 2018 formulary (biopharmadive.com)
Express Scripts, a top-three pharmacy benefit manager in the U.S., will exclude an additional 64 drugs from its national listing of preferred drugs next year, sending shares in several biotechs affected spinning...Notably, the PBM's 2018 formulary leaves off Amgen's neutropenia blockbuster Neupogen (filgrastim) in favor of Novartis' biosimilar medicine Zarxio (filgrastim-sndz) and drops Lilly's osteoporosis drug Forteo (teriparatide)...Forty-six other brand-name drugs with generic competitors already on the market were also excluded, potentially accelerating uptake of cheaper copies. Valeant Pharmaceuticals, in particular, could see an impact as two of its top-three best-selling drugs were shut out from Express Script's preferred list...Express Scripts has been an outspoken critic of drugmakers' pricing practices, frequently pushing back against the pharma industry's attempt to pin the blame for rising costs on the rising power of PBMs...Express Scripts' newly released formulary for next year substantially increases the number of drugs excluded by the PBM to a total of 159. The PBM was quick to highlight, however, that the new exclusions would only affect 0.67% of its members while saving cash overall...
- Will CVS Health’s Point-of-Sale Rebates Deflate the Gross-to-Net Bubble—and Disrupt the PBM Business? (drugchannels.net)
I examined the magnitude of the gross-to-net bubble—the growing spread between a manufacturer’s list price for a drug and the net price to a third-party payer after rebates...The bubble directly affects patients’ out-of-pocket costs. Many patients now have benefit plans with deductibles and are therefore required to pay the full, undiscounted cost of their prescriptions. Patients taking specialty drugs face large coinsurance computed using the undiscounted list price...One solution replaces formulary payments made to plan sponsors with prescription discounts for patients at the point of sale. Last week, CVS Health became the first pharmacy benefit manager to publicly embrace and explain this alternative benefit design...Do point-of-sale rebates solve the patients’ problems that the gross-to-net bubble causes? And will this benefit design mark the beginning of the end for the PBMs’ traditional economic model?