- Debate Intensifies Over Express Scripts Future As Standalone PBM (forbes.com)
A debate has emerged over the future of the standalone pharmacy benefit manager, putting Express Scripts at the center of an intensifying discussion over how best to manage drug costs for consumers, employers and the government...Pharmacy benefit managers are middlemen between drug makers and consumers when it comes to purchasing drugs and providing prescription coverage...PBM’s role has come under scrutiny lately as high priced drugs bust employer and government budgets for prescriptions. Critics are questioning whether PBMs operate in a transparent way and therefore don’t pass along all of the savings they can to consumers...insurers are closing ranks around a model that brings the PBM closer to the health insurer. UnitedHealth Group owns OptumRx, a rapidly growing PBM and Anthem is seeking requests for proposals from PBMs for a new contract that would begin in 2020. Anthem's current contract with Express Scripts runs out at the end of 2019...Express Scripts, however, says it has a track record of saving Anthem and its employer clients money and is committed to the standalone model...
- NCPA Asks U.S. Senate and House Leadership to Hold Hearings on Pharmacy DIR Fees Bills (ncpanet.org)
The National Community Pharmacists Association recently requested Congressional hearings on legislation, the Improving Transparency and Accuracy in Medicare Part D Spending Act, that would stop the unfair practice of pharmacy direct and indirect remuneration (DIR) fees being applied retroactively under Medicare Part D...Retroactive pharmacy DIR fees are creating a system of winners and losers...While pharmacy benefit managers profit, the unpredictable timing and amount of these clawbacks are wreaking financial havoc on pharmacies, seniors, and taxpayers...By requiring PBMs to divulge the costs of prescription drugs for Medicare beneficiaries at the point of sale, these bills fix a problem even the Centers for Medicare & Medicaid Services acknowledges has contributed to rising costs in Medicare Part D.
- DIR fees are pushing seniors into the donut hole coverage phase faster, where seniors absorb all of the costs for their prescriptions;
- DIR fees are also pushing seniors into the ensuing catastrophic coverage phase faster, where the government's costs have risen from $10 billion in 2010 to $33 billion in 2015;
- In both of those instances, the PBMs' co-pay burden disappears, which is not the case in the initial phase of coverage;
- Independent community pharmacies' ability to plan in advance is being undermined by how PBMs currently apply DIR fees, threatening patient access to these pharmacies, especially in underserved communities; and
- All of this is occurring while PBMs continue to operate in a non-transparent manner when it comes to DIR fees.
- You’re Overpaying for Drugs and Your Pharmacist Can’t Tell You (bloomberg.com)
Eric Pusey has to bite his tongue when customers at his pharmacy cough up co-payments far higher than the cost of their low-cost generic drugs, thinking their insurance is getting them a good deal...Pusey’s contracts with drug-benefit managers at his Medicap Pharmacy in Olyphant, Pennsylvania, bar him from volunteering the fact that for many cheap, generic medicines, co-pays sometimes are more expensive than if patients simply pay out of pocket and bypass insurance. The extra money -- what the industry calls a clawback -- ends up with the benefit companies…Clawbacks, which can be as little as $2 a prescription or as much as $30, may boost profits by hundreds of millions for benefit managers and have prompted at least 16 lawsuits since October. The legal cases as well dozens of receipts obtained by Bloomberg and interviews with more than a dozen pharmacists and industry consultants show the growing importance of the clawbacks.
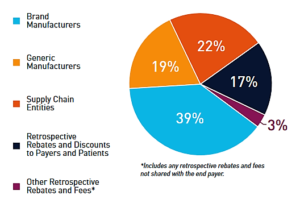
- PhRMA-backed report analyzes ‘complex process’ of drug pricing (biopharmadive.com)
The PhRMA-backed report made the case that drugmakers are not solely to blame for ballooning treatment prices, which have come under intense scrutiny from state and federal legislatures, industry executives and research organizations...As competition in the pharmaceutical marketplace has increased in recent years, brand manufacturers have been making larger payments for market access to their medicines...Government-mandated discounts and fees have also increased over the last five years. Many of these discounts are not plainly visible, leading to misperceptions about the relative share of gross and net drug expenditures realized by brand manufacturers...each player has taken home large chunks of the drug sales revenue as well...non-manufacturers, which include wholesalers, PBMs, health plans and pharmacies, snag 42% of gross drug spending — which doesn't take into account any type of discount — from the initial point-of-sale payment for a drug by a payer or patient...Branded drugmakers take home 39% of those gross expenditures, with generics manufacturers gobbling up 19%...
- In the debate over rising drug prices, both drugmakers and PBMs claim innocence (cnbc.com)
The battle over rising drug prices has become a full-blown he-said-she-said...Drug companies have pointed the finger at middlemen in the health-care system, saying they not only benefit from rising drug prices but contribute to their increases...Those middlemen — namely, pharmacy benefits managers (or PBMs) — have said the only parties responsible for drugs' list prices are the manufacturers...So who's right?...In a study released today, the PBM lobbying group, the Pharmaceutical Care Management Association, says an analysis it commissioned revealed no correlation between drug prices and rebates paid back to PBMs...The drug industry's lobby, the Pharmaceutical Research and Manufacturers of America...disagrees...
- Drug Costs Too High? Fire the Middleman (bloomberg.com)
Caterpillar’s lowered drug bills show why pharmacy benefit managers are under fire. A decade ago, Caterpillar Inc. looked at its employee drug plan and sensed that money was evaporating... By hiring its own doctors and pharmacists, among other changes, Caterpillar has saved tens of millions of dollars a year...The model is as successful today as it’s ever been...Caterpillar’s move away from benefit managers started when it suspected that as much as a quarter of its $150 million drug spending was wasted. The company devised its own list of drugs to offer its U.S. health-plan members and negotiated deals with pharmacies. It promoted generics and discouraged use of expensive heartburn and cholesterol medicines. The changes have saved the company $5 million to $10 million per year on cholesterol-lowering statins alone...Drug spending at Caterpillar...has dropped per patient and per prescription since the company started the program...
- Drug Benefit Managers Need More Oversight, Pharmacists Say (bloomberg.com)
Middlemen who manage drug benefits for employers and insurers should be under greater government oversight of their pricing and billing practices to make health care cheaper, an independent pharmacists’ group said (National Community Pharmacists Association)...plans to lower prescription drug costs will only succeed if greater transparency is imposed on pharmacy benefit managers...Benefit managers engage in price negotiations that are often kept secret for competitive reasons, with manufacturers on one end and pharmacies on the other. Pharmacists have criticized these discussions, as well as so-called clawbacks -- extra profit for the PBM after co-pays for cheap, generic medicines exceed the price of the drug itself...PBMs...continue to operate in a virtual black box...As the outcry over drug pricing intensifies, the middlemen have gained more attention...
- New PBM programs bypass insurers to offer drug discounts directly to consumers (modernhealthcare.com)
Pharmacy benefit managers and tech startups are responding to underinsurance and the onslaught of high-deductible health plans by cutting out insurers in the quest to help patients lower their prescription drug costs...Two PBMs have launched discount programs for patients to use outside of any insurance coverage they might have. It's a notable contrast to PBMs' main business serving as third-party administrators of prescription drug coverage for insurers and employers...These efforts come as a budding industry has sprung up around helping consumers and employers rein in prescription drug costs. Startups like Blink Health and RefillWise offer pharmacy cards that provide consumers with negotiated discounts if they don't use their prescription coverage, while some insurers and pharmacy benefit managers, along with tech firm Castlight Health, are attempting to allay consumer and employers' concerns about drug costs by building apps that offer price transparency to physicians or patients.
- Obamacare plans’ drug spending rose faster than other plans in 2016: Express Scripts (in.reuters.com)
Spending on prescription drugs for health plans created under the Affordable Care Act increased last year at a rate more than three times that of other commercial plans and most government-run plans managed by Express Scripts Holding Co...year-over-year spending per person for individual insurance plans sold on the Obamacare exchanges where it manages the pharmacy benefit rose 14 percent in 2016, driven by higher drug prices and utilization...Express Scripts said per-capita spending for other commercial plans it manages, mostly for employers, rose just 3.8 percent last year, despite an 11 percent increase in list prices for brand-name drugs...Drug spending for plans the company manages under Medicare...increased 4.1 percent last year while the rise for Medicaid...was 5.5 percent.
- Express Scripts Reveals What Really Drives Drug Spending—And Why the Government May Do No Better (drugchannels.net)
Last week, Express Scripts released its 2016 Drug Trend Report for the commercial market…For 2016, drug trend—the year-over-year change in spending—was a mere 3.8% for Express Scripts’ commercial plan sponsor customers. The Express Scripts data also highlight how drug prices were only part of the reason behind moderating drug spend. Contrary to the public rhetoric, increased utilization was a bigger influence than higher prices for both specialty and traditional drugs...The new Express Scripts report deconstructs year-over-year changes in drug spending into its two primary components:
- Unit costs—the payer’s cost per unit of therapy. Unit costs vary with: 1) the rate of inflation in brand-name drug prices, 2) shifts to different drug options within a therapeutic class, 3) a shift in mix of therapeutic classes utilized by beneficiaries, and 4) the substitution of generic drugs for brand-name drugs. Note that for the second year in a row, the Express Scripts unit cost data account for the value rebates shared with payers.
- Utilization—the total quantity of drugs obtained by a payer’s beneficiaries. Utilization varies with: 1) the number of people on drug therapy, 2) the degree to which people adhere to their drug therapy, and 3) the average number of days of treatment.