- Drugmakers Split on Whether to Include Interchangeability Statement in Biosimilar Labels (raps.org)
Drug, biologic and biosimilar companies’ comments on Food and Drug Administration draft guidance on biosimilar labeling reveals a major split between those who do and do not want a statement on a biosimilar’s interchangeability status on each new product's label...FDA has still yet to release its guidance on what interchangeability means, and as FDA has not found any biosimilar to be interchangeable with its reference product…
- Amgen says it...believes a biosimilar label should include a summary of the clinical data, including immunogenicity data, used to demonstrate biosimilarity or interchangeability…
- Pfizer said...biosimilars should not be labeled "as though they were small molecule generic drugs" and that it "recommends that biosimilar labeling include a statement reflecting whether interchangeability has been assessed."
- Merck & Co...says "that a single blanket approach applicable to all biosimilar products is not appropriate, and may cause unnecessary confusion among stakeholders."...recommends that rather than using such blanket statements, FDA take a risk-based approach for each biosimilar…
- Boehringer Ingelheim says that it "does not agree that a biosimilar label needs to include a ‘biosimilarity statement,’...Such information is not ‘essential scientific information needed by health care practitioners for the safe and effective use of a drug.’
- Sandoz...says... "It is self-evident that the very act of highlighting the indications that are extrapolated is being proposed by some groups in order to raise doubts as to the safety and efficacy of the biosimilar for those indications, and perhaps to also imply inferiority of biosimilars across the board.
- Most Californians support a measure to obtain state discounts on drugs (statnews.com)
The pharmaceutical industry may be losing a heated battle over drug prices in California...A poll released earlier this week found that two-thirds of Californians support an initiative that would require drug makers to offers discounts to state health programs…At issue is the California Drug Price Relief Act (Proposition 61), which would revise state law to require the state Medicaid program, which is known as Medi-Cal, and other state programs to pay no more for medicines than the prices negotiated by the US Department of Veterans Affairs. Currently, the VA gets a 24 percent discount off average manufacturer prices...The measure is being closely watched as a litmus test for public discontent over prescription drug costs and the extent to which such efforts may crop up in other states, a point of great importance to drug makers. So far, the only state where a similar initiative is being organized is Ohio...California is often seen as a bellwether state for political trends and voter attitudes...
- EU regulators say China’s Jinan Jinda still missing manufacturing mark (fiercepharma.com)
When EU regulators last year came down on China’s Jinan Jinda Pharmaceutical for slipshod manufacturing work, the company brought in a U.S. consultant to get its Zhangqiu, Shandong, plant in order. But a recent follow-up found that Jinan Jinda continues to ship its antibiotic to some European customers even though its improvement efforts fall short of what they need to be...the European Directorate for the Quality of Medicines said it has been recommended that Jinan Jinda's nitrofurantoin antibiotic be banned from the EU and that the plant's certificate of compliance be suspended, or even "voided."...The investigators reported that there were critical deficiencies in the way the plant handled raw data safety, control and out-of-specification reviews. There were major deficiencies in training, change control, quality assessment, process and cleaning validations.
- Pharmacy benefit managers are restricting access to lots of drugs next year (statnews.com)The ‘gouge factor’: Big companies want transparency in drug price negotiations (statnews.com)
In the latest bid to control prescription drug spending, the nation’s largest pharmacy benefits managers are again excluding dozens of medicines from their lists of products that are covered by health insurance…Express Scripts notified its customers that next year, 85 medicines will be excluded from its national formulary, and, as a result, the PBM hopes to recognize about $1.8 billion in savings, up from $1.3 billion this year. The number of excluded medicines, by the way, is down slightly from the 88 prescription drugs that were excluded from its 2016 formulary...CVS Health released its own 2017 formulary that will exclude another 35 medicines, including 10 that were called "hyperinflationary." As a result, CVS is now excluding a total of 131 medicines and boasts such moves have saved more than $9 billion over the last five years…Recently, a group of two dozen of the largest names in Corporate America — including Macy’s, Coca-Cola and American Express — formed an alliance (Health Transformation Alliance) to find ways to lower health care costs. One notion they are exploring is to change the way PBMs are paid due to concerns that the rebates the PBMs collect from drug makers on behalf of clients are not always passed along. The PBMs have disputed this argument.
- Drug lobby plans counterattack on prices (politico.com)
It is just one part of a larger effort by the K Street powerhouse to seize control of the public narrative over drug prices...Washington’s powerful drug lobby is gearing up to spend hundreds of millions of dollars on a post-election ad war pushing back against politicians from both parties who have savaged its members over drug prices...The massive campaign by the Pharmaceutical Research and Manufacturers of America — expected to start positive by highlighting drugs that save or prolong lives — will dwarf the $20 million that health insurers spent on the iconic "Harry and Louise" campaign credited with sinking Hillary Clinton's health reform plan in the early 1990s.
- Noted price-hiker Jazz feels the heat as PTO strikes Xyrem patents (fiercepharma.com)
Jazz Pharmaceuticals has been called out repeatedly for substantial price hikes on its leading product Xyrem. But now, the company’s cash cow could be in trouble...the...drugmaker saw four patents on its most important asset upturned by the U.S. Patent and Trademark Office, through the inter partes review system pharma has come to dread. The PTO is due to rule on two more "imminently,"...and given their similarity to those already tossed, they could well suffer the same fate...The patent loss is a blow to...Jazz, whose narcolepsy star generates more than 70% of its operating profit...The med has grown to that point somewhat controversially, as Jazz hiked its list price 841% over the 5 years ending in 2013.
- Rogue online sellers feeding drug abuse (chaindrugreview.com)Internet Drug Outlet Identification Program Progress Report for State and Federal Regulators: July 2016 (s3.amazonaws.com)
Drug abuse, including misuse of prescription drugs, remains at alarmingly high levels...Feeding this epidemic, the National Association of Boards of Pharmacy says, are rogue Internet drug outlets illegally dispensing prescription controlled substances...illicit online drug sellers "hiding behind sleek websites" are making it easier for people struggling with drug abuse to purchase controlled-substance medications. However, since these rogue websites often sell counterfeit and tainted substances, buyers can raise the risk of overdose and death...researchers used popular search engines (Google, Bing and Yahoo), shopping websites (eBay, Craigslist, Yahoo! Shopping, Overstock.com, Etsy, Oodle, eCRATER, Bonanza, Sell.com, Blujay and Alibaba) and social media sites (YouTube and Twitter) to gauge the availability of the opioids Demerol, Dilaudid, Duragesic, Exalgo, Kadian, Lorcet, Lortab, Percocet, Roxicet, Vicodin and Zohydro. Opioids were easiest to find and readily available by using search engines, the researchers discovered. Still, no matter which online avenue was used, researchers found that the final destination was a dedicated website selling opioids illegally.
- Express Scripts bars new launches from Lilly, Merck and shuts out Novo for 2017 (fiercepharma.com)
For the third year in a row, Express Scripts unveiled a new national formulary excluding dozens of drugs. And for the third year in a row, a short list of winners and losers comprises some of Big Pharma’s biggest launches...The list of excluded meds--85 for 2017--covers many of the same brand names as before. For instance, Novo Nordisk’s blockbuster GLP-1 diabetes drug Victoza and two of its top-selling insulins remain barred, as Express Scripts favors Eli Lilly’s diabetes range--and most likely, Lilly’s discounts. AbbVie’s hepatitis C cocktails Viekira Pak and Technivie remain the chosen therapies in that field, with Gilead Sciences' first-to-market meds Harvoni and Sovaldi out in the cold...Express Scripts and its biggest pharmacy benefits rival, CVS Health, started the exclusionary formulary trend a few years ago by kicking off a handful of meds that they saw as too costly and easily replaced...Express Scripts continued its tradition of punishing drugmakers that have pushed through big price hikes, used co-pay discount cards to hawk me-too meds, and employed other strategies the PBM considers no-nos.
- Implications of final AMP rule for community Rx (chaindrugreview.com)
On February 1, 2016, the Centers for Medicare & Medicaid Services released its Final Rule interpreting the provisions of the 2010 health care reform law that address the Medicaid Drug Rebate Program. While much of the Final Rule speaks to drug manufacturer rights and responsibilities in the MDRP, significant portions are directly applicable to chain drug stores...the Final Rule addresses (a) reimbursement for multisource drugs dispensed to Medicaid patients, (b) changes in the Average Manufacturer Price (AMP) that will impact pharmacy reimbursement for multisource products, (c) reimbursement for single-source drugs dispensed to Medicaid patients and (d) changes to the dispensing fees pharmacies will receive for dispensing drugs to Medicaid patients...An overarching theme expressed in the Final Rule is CMS’ desire to move states away from their historic practice of overpaying for ingredient cost while simultaneously underpaying for dispensing fees...If the Final Rule plays out as anticipated, in the coming year ingredient cost reimbursement will fall for single- and multiple-source products, but dispensing fees will rise...This reflects a desired shift away from a "spread-based" model of pharmacy Medicaid participation toward a "service-based" model. It’s currently unclear if the increased fee income to pharmacies will balance the lost reimbursement revenue.
- Multisource product ingredient cost reimbursement
- Changes in AMP affecting multisource drug reimbursement
- Single-source product ingredient cost reimbursement
- Medicaid pharmacy dispensing fees
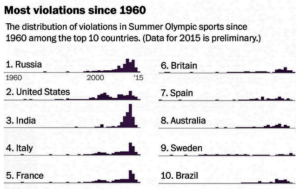
- What banned drugs do cheating athletes take? (washingtonpost.com)
Hundreds of substances are named on the World Anti-Doping Agency’s list of banned drugs, and thousands more are prohibited through phrases such as "and related substances." That way, the rules cover drugs that may not have been detected or even invented yet...Most, but not all, fall into these broad categories:
- Muscle-building steroids
- Pick-me-up stimulants
- Hormones and drugs that modulate hormones
- Drugs that hide other drugs
- Calming beta blockers
- Asthma drugs
- Recreational drugs
- Anti-inflammatory steroids
- Other ways to break the rules