- ICER to Work With VA on Drug Price Negotiations (raps.org)
In a first for the Institute for Clinical and Economic Review, which estimates the cost-effectiveness of drugs, the Department of Veterans Affairs Pharmacy Benefits Management Services office has agreed to use ICER drug assessment reports in drug coverage and price negotiations with the pharmaceutical industry...ICER says it will work with staff in the VA to integrate ICER reports into the VA formulary management process of evaluating the comparative clinical effectiveness and value of drugs...The VA requires that drug manufacturers offer a 24% discount off a drug’s average price or the lowest price paid by other (nonfederal) buyers, in addition to further discounts if a drug’s price outstrips inflation...The VA also directly negotiates lower prices with drug manufacturers, and with ICER’s help may establish a new norm for how the government can obtain lower-priced drugs...We will also assist the VA in exploring new ways it can use the reports to continue to provide a safe, effective and sustainable prescription benefit while more closely aligning a drug’s price with the value it provides to Veterans and the US taxpayer...ICER will also work with VA staff to develop options for using "value-based price benchmarks"...
- This Week in Managed Care: July 7, 2017 (ajmc.com)
Kelly Davio, Welcome to This Week in Managed Care from the Managed Markets News Network
- Endo to pull opioid painkiller off U.S. market after FDA nudge (reuters.com)
Endo International Plc agreed...to remove its long-acting opioid painkiller from the U.S. market to comply with the health regulator's request last month, sending its shares down as much as 3 percent...The U.S. Food and Drug Administration in June had requested the withdrawal of Endo's Opana ER, marking the first time the agency asked for an opioid painkiller to be taken off the market for public health reasons...The regulator's request followed the recommendation of an independent panel of advisers, which concluded that the drug's benefits no longer outweighed its risks...
- This Week in Managed Care: June 30, 2017 (ajmc.com)
Kelly Davio, Welcome to This Week in Managed Care from the Managed Markets News Network
- Change law and raise taxes to enable STPs to improve NHS, report urges (pharmaceutical-journal.com)
A lack of statutory power and severe underfunding are creating barriers to promising NHS reforms set out in sustainability and transformation plans (STPs), a think tank is warning...A report from the Institute for Public Policy Reform found that...44 regions in England had by and large correctly identified the right solutions, including moving care into the community and prevention...But there are several barriers that will prevent the ‘vision’ being realised, including a failure of leadership, the risk the NHS is being ‘engulfed by funding pressures’ and a lack of legal power to deliver the reform set out by the STPs...Among the IPPR recommendations is a call for the government to create a new ‘NHS tax’ by raising taxes for the highest paid to provide an extra £3.9bn a year to tackle the NHS ‘funding crisis’...In coming years, the NHS is facing a £22bn funding gap, which means limited resources are being spent maintaining the status quo rather than introducing a reform…There should also be changes to the law to better enable the pooling of budgets and commissioning functions locally and to give regional bodies a formal role in the system and put into effect place-based health and care...
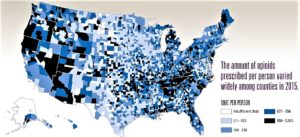
- Opioid prescribing is falling in the US, but not everywhere (philly.com)
Centers for Disease Control and Prevention...Prescriptions per capita, measured in morphine equivalents to account for various strengths and drug types, have declined steadily since their 2010 peak...Half the nation’s counties saw a decline (a quarter were stable) from 2010 to 2015. But there was wide variation, with providers in the highest-prescribing counties writing scripts for six times more opioids per resident than those in the lowest-prescribing counties...Nationally, the epidemic has been driven by high rates of addiction in more rural and white areas...Looking at county-level prescribing data helped CDC researchers to shed more light on some patterns of the painkiller epidemic. Counties with high rates tended to:
- Contain small cities or large towns (perhaps with pharmacies that drew residents from rural areas)
- Have higher percentages of white residents
- Have more dentists and primary-care physicians per capita
- Have more residents who were uninsured or unemployed
- Have more people with diabetes, arthritis, or a disability
But county-by-county analyses also illustrated how much is unknown about where and why opioids are given.
- Residents in 14 Nevada Counties Will Not Have Access to Qualified Health Plans (ktvn.com)
The Division of Insurance has announced that Nevada’s insurance carriers that participate in the Silver State Health Insurance Exchange have decided to only offer coverage to Clark, Washoe, and Nye counties beginning in 2018...Currently three medical carriers offer plans on Nevada Health Link:
- Anthem (The only insurance company currently selling statewide)
- Health Plan of Nevada
- Prominence Health Plan
But some changes are coming as of January 1, 2018.
- Anthem & Health Plan of Nevada will only be offering coverage in Washoe, Clark, and Nye Counties.
- Prominence Health Plan announced this week that they will be pulling out of the Nevada Exchange market.
- Two new companies, Aetna and Centene will be joining the exchange market but according to the Division of Insurance at most they will only be offering plans in Washoe, Clark, and Nye counties
The Division of Insurance says this will leave about 8,000 Nevada residents without coverage across 14 counties. The largest group is about 5,000 people across Carson City, Douglas, Lyon, and Storey Counties...If you live outside of Washoe, Clark, or Nye counties and have concerns about your coverage, Silver State Health Exchanges suggests you call them at 855-768-5465...They say that they are working diligently with Governor Sandoval to come up with a plan for those that could be uninsured.
- Pharmacy Week in Review: July 7, 2017 (pharmacytimes.com)
Nicole Crisano, PTNN. This weekly video program provides our readers with an in-depth review of the latest news, product approvals, FDA rulings and more.
- Walgreens, Rite Aid end $9.4 billion merger (pharmacist.com)
Walgreens Boots Alliance and Rite Aid have called off their $9.4 billion merger agreement. Instead, Walgreens says it will attempt to purchase one-half of Rite Aid's stores for $5.18 billion in cash. Executives said they crafted the smaller deal to address regulatory issues, but antitrust experts said it does not eliminate competition concerns. The Federal Trade Commission's review of the original Walgreens-Rite Aid transaction stretched 18 months, and the commission reportedly did not back away from concerns that the deal would have harmed competition. The commission worried about the merger's impact in regions where both companies have a strong store presence...Walgreens...said the smaller transaction addresses "all substantive" FTC concerns. The company will be adding stores in regions where it currently lacks a large presence, including the Northeast and MidAtlantic..."There's a chance that it won't go, that's the reality of the process. We believe it makes sense, we just have to wait until it plays out."
- Proposed Health Insurance Rate Changes for Exchange Released (ktvn.com)Additional information on proposed rate changes can be accessed by visiting the Division's website (healthrates.doi.nv.gov)
There will be four insurance companies offering insurance plans on the Exchange with a total of 24 individual health plans to choose from between Clark, Washoe and Nye counties in 2018...The Nevada Division of Insurance has posted a summary of proposed rate changes for Plan Year 2018 on the Division’s website. These proposed rate changes are for plans sold on the Nevada’s health insurance Exchange in the individual market..."Posting these rate changes on the website allows the Division to be transparent with Nevada’s consumers so that they have an opportunity to review these requests from insurance carriers," said Insurance Commissioner Barbara Richardson. "This is also an opportunity for consumers to submit their comments to the Division during this rate review process."...The average proposed rate change for the individual market on Exchange is an increase of 38%.